Could sugar self-substitution for opioids in our patient’s be leading to insulin resistance, obesity, T2DM?
In an experiment done on mini-pigs, they found that sugar can affect the brain’s reward system in a similar “manner similar to that of drugs of abuse”
Sugar’s impact on the brain’s reward system boils down to how it affects two types of receptors in the brain.
The first set is dopamine receptors — dopamine is a central player in the brain’s reward system, released during pleasurable activities.
The second set is opioid receptors, which are also found all over the brain but are particularly found in areas involved in eating-related rewards.
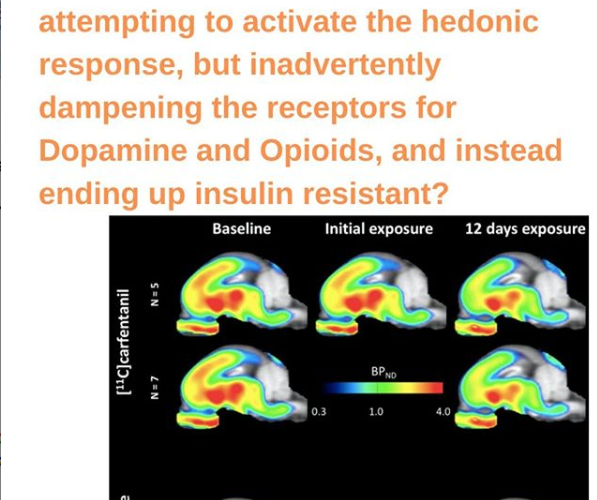
The sensitivity of both receptors was dampened when pigs were allowed unrestricted access to sugar water for one hour each day for twelve days. The pigs were also fed a normal diet, so sugar consumption was unrelated to their caloric needs.
After the first day, the sugar intake lowered the “availability” of opioid and dopamine receptors, essentially dampening the ability of these receptors to bind to their natural ligands. Both Opiate and Dopamine receptor binding was attenuated 14% in the anterior cingulate cortex and the nucleus accumbent, both are areas of the hedonic reward.
At the end of the 12 days, the scientists found that the pattern held — the availability of both types of receptors continued to decrease significantly.
Could sugar self-substitution for opioids in our patient’s be leading to insulin resistance, obesity, T2DM?
Winterdahl, M., Noer, O., Orlowski, D. et al. Sucrose intake lowers μ-opioid and dopamine D2/3 receptor availability in porcine brain. Sci Rep 9, 16918 (2019) DOI:10.1038/s41598-019-53430-9.